The DSM
por Kimberley Croft
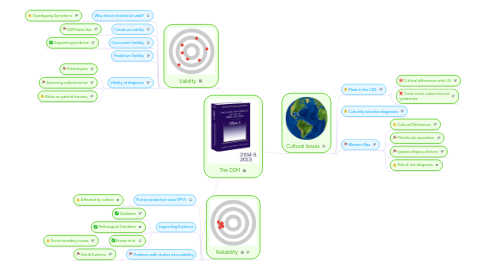

1. Validity
1.1. Why does it need to be valid?
1.1.1. Overlapping Symptoms
1.2. Construct validity
1.2.1. DSM lacks this
1.3. Concurrent Validity
1.3.1. Supporting evidence
1.4. Predictive Validity
1.5. Validity of diagnosis
1.5.1. Stereotypes
1.5.2. Assuming cultural norms
1.5.3. Relies on patient honesty
2. Reliability
2.1. Postive predictive value (PPV)
2.1.1. Affected by culture
2.2. Supporting Evidence
2.2.1. Goldstein
2.2.2. Pathological Gamblers
2.2.3. Brown et al.
2.2.3.1. Some boundary issues
2.3. Problems with studies into reliability
2.3.1. Kirk & Kutchins
3. Cultural Issues
3.1. Made in the USA
3.1.1. Cultural differences with US
3.1.2. Omits some culture-bound syndromes
3.2. Culturally sensitive diagnoses
3.3. Western Bias
3.3.1. Cultural Differences
3.3.2. Mind-body separation
3.3.3. Ignores religious factors
3.3.4. Risk of mis-diagnosis
