1. Age and Gender most likely to occur in
1.1. Adolescents and young women
2. Strategies for Detection
2.1. 2 types of Anorexia
2.1.1. Restricting
2.1.1.1. Low Calorie Count
2.1.1.2. Eating only one meal a day
2.1.1.3. Obsessive/ Rigid Eating Rules
2.1.2. Purging
2.1.2.1. Vomiting or Diarrhea
2.1.2.1.1. Using diet pills, laxatives, diuretic
2.1.2.2. Throwing up after eating
2.1.2.3. Compulsive Exercising
2.2. Food Behaviour
2.2.1. Dieting
2.2.2. Obsession with calories
2.2.3. Pretending to eat or lying
2.2.4. Preoccupation with food
2.2.5. Strange food rituals
2.2.6. Avoidance of social situations involving food
2.2.7. Denial of hunger
2.3. Appearance and Body Image
2.3.1. Dramatic weight loss
2.3.2. Feeling fat despite being underweight
2.3.3. Obsessed with body image
2.3.4. Critical of self appearance
2.3.5. Denial of being too thin
3. Social Implications
3.1. Culture and values about being thin
3.1.1. Media/TV
3.1.1.1. Images of "Perfect Body"
3.1.1.1.1. Celebreties
3.1.2. Valuing people according to appearance
3.1.3. Family
3.1.3.1. Over controlling parents
3.1.3.1.1. Pressure
3.1.3.2. Troubled family relationships
3.1.3.3. Divorce/separation
3.1.4. Stressful Life events
3.1.4.1. Break ups
3.1.4.2. Puberty
3.1.4.3. Leaving home
3.1.4.4. Sexual and physical abuse
3.1.5. Society
3.1.5.1. Low socioeconomic
3.1.5.1.1. Less resources
3.1.5.2. Homosexual community
3.2. Pressures to succeed
3.3. Professions relating to body image/types
3.3.1. Fitness Instructor
3.3.2. Models/TV Person/Celebreties
3.4. Peer Pressure
3.4.1. Being bullied
3.5. Isolation/lonliness
4. Ethical Implications
4.1. Disorder controlled by the individual
4.2. Refusal of treatment
4.2.1. Force feeding
4.2.1.1. Unethical
4.3. Severity of the symptoms
4.3.1. When or when not to treat?
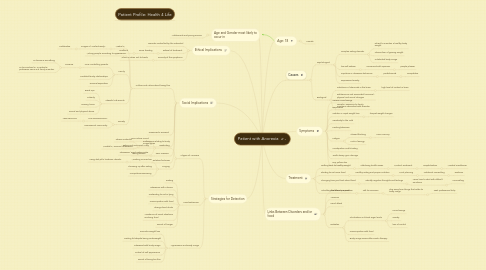
5. Patient Profile: Health 4 Life
6. Age: 18
6.1. Female
7. Causes
7.1. Psychological
7.1.1. complex eating disorder
7.1.1.1. refusal to maintain a healthy body weight
7.1.1.2. Intense fear of gaining weight
7.1.1.3. a distorted body image
7.1.2. low self esteem
7.1.2.1. concerned with opinions
7.1.2.1.1. people pleaser
7.1.3. impulsive or obsessive behaviour
7.1.3.1. perfectionists
7.1.3.1.1. competitive
7.1.4. Depression/anxiety
7.2. Biological
7.2.1. imbalance of chemicals in the brain
7.2.1.1. high level of cortisol in brain
7.2.2. adolescence and associated hormonal, physical and neural changes
7.2.3. Genetic- exposure to family members associated with disorder
8. Symptoms
8.1. Severe mood swings
8.2. Depression
8.3. Sudden or rapid weight loss
8.3.1. frequet weight changes
8.4. Sensitivity to the cold
8.5. Fainting/dizziness
8.6. Fatigue
8.6.1. Slowed thinking
8.6.1.1. Poor memory
8.6.2. Lack of energy
8.7. Constipation and bloating
8.8. Tooth decay, gum damage
8.9. Dry, yellow skin
9. Links Between Disorders and/or food
9.1. Low Blood pressure
9.2. Aneamia
9.3. Heart attack
9.4. Diabetes
9.4.1. Fluctuations in blood sugar levels
9.4.1.1. mood swings
9.4.1.2. anxiety
9.4.1.3. loss of control
9.4.2. Preoccupation with food
9.4.3. Body Image issues after insulin therapy
10. Treatment
10.1. Getting back to healthy weight
10.1.1. Stabilising health issues
10.1.1.1. Medical Treatment
10.1.1.1.1. Hospitalisation
10.2. Starting to eat more food
10.2.1. Healthy eating and proper nutrition
10.2.1.1. Meal planning
10.2.1.1.1. Nutitional counselling
10.3. Changing how you think about food
10.3.1. Identify negative thoughts and feelings
10.3.1.1. Learn how to deal with difficult emotions
10.3.1.1.1. Counselling
10.4. Admitting that there is a problem
10.4.1. Talk to someone
10.4.1.1. Stay away from things that relate to body image
10.4.1.1.1. Seek professional help
