1. Mouth
2. Mouth: PQRST
2.1. Sores/Lesions
2.2. Sore throat
2.3. Bleeding gums
2.4. Toothache
2.5. Hoarseness
2.6. Dysphagia
2.7. Altered taste
2.8. Smoking/alcohol use
2.9. PCC: dental care and
3. Mouth: Objective Data
3.1. Inspection:
3.2. Lips for color, moisture, cracking, lesions
3.3. Teeth and gums: missing teeth and gum health is indicative of general health
3.4. Tongue: color, surface, moisture, not patches/lesions
3.5. Uvula: midline and moves (CN 10)
4. Mouth Abnormalities
4.1. Cleft lip
4.1.1. Maxillaryfacial cleft common with congenital deformities
4.1.1.1. Family history, drug use, alcohol
4.2. Herpes Simplex (HSV 1)
4.2.1. Virus
4.2.1.1. Common cold sore
4.2.1.1.1. Clear vesicles, evolve to pustules, and crust
4.3. Ginigvitis
4.3.1. Gum margins red and swollen
4.3.1.1. Bleed easily
4.3.1.1.1. Diabetes, pregnancy, poor oral hygiene
4.4. Gingival hyperplasia
4.4.1. Painless enlargement of the gums
4.4.1.1. Puberty, pregnancy, leukemia
4.5. Ulcers
4.5.1. Canker sores
4.5.1.1. Painful
4.5.1.1.1. Last 1-2 weeks
4.6. Candidiasis
4.6.1. White, cheesy, curd, like
4.6.1.1. Thrush
4.6.1.1.1. An opportunist infection more common in immunocompromised such as HIV
4.7. Ankyloglossia
4.7.1. Short lingual frenulum
4.7.1.1. Tongue tie
4.7.1.1.1. Effects speech, and limits mobility
4.8. Black hairy tongue
4.8.1. Overgrowth of mycelial threads from fungus infection
4.8.1.1. Can occur after use of antibiotics
4.8.1.1.1. Heavy smoking may be a contributing factor
4.9. Carcinoma
4.9.1. Ulcer with rolled edges
4.9.1.1. Indurated (hard)
4.9.1.1.1. Risk for metastasis
5. The Aging Adult
5.1. Nose may appear prominent
5.2. Teeth may be slightly yellow
5.3. Gum margins may be receded
5.4. Dental deterioration/ loss of teeth
5.5. Diminished taste
5.6. Decreased salivation
5.7. Trouble with mastication
6. Culture and genetics
6.1. Bifid Uvulua:
6.1.1. American indians
6.2. Cleft lip/palate:
6.2.1. Asians, whites and least in Blacks
6.3. Dental caries:
6.3.1. Low socioeconomic status
6.3.1.1. Lack of access to healthcare
6.4. Periodontal disease:
6.4.1. Type 2 DM
6.5. Oral cancer:
6.5.1. HPV, tobacco use
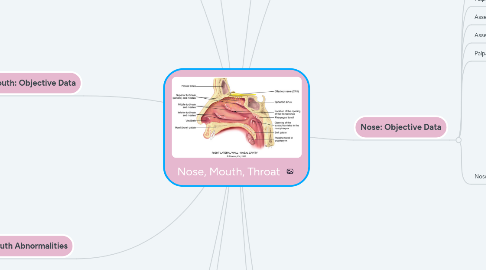
7. Nose
7.1. Divided by septum
7.2. Olfactory receptors (CN 1)
7.3. Hair cells (cilia)
7.4. Sinuses : air-filled pockets
7.4.1. Using thumbs, press frontal sinuses by pressing up and under the eyebrows and over maxillary sinuses below cheekbones.
7.4.2. Transillumination
7.4.3. You may use this technique when you suspect sinus inflammation, although it is of limited usefulness.
7.4.4. Darken room; affix strong narrow light to end of otoscope and hold it deep under superior orbital ridge against location of frontal sinus area; cover with your hand.
7.4.5. A diffuse red glow is a normal response; it comes from light shining through air in the healthy sinus.
7.5. Lighten weight of skull bone, resonate sounds, provide mucus
7.6. When inflamed results in sinusitis
8. Nose PQRST
8.1. Discharge
8.1.1. Rhinorrhea: runny nose
8.1.1.1. Clear, yellow, green, bloody?
8.2. Frequent URI’s
8.3. Sinus pain
8.4. Trauma
8.5. Epistaxis
8.5.1. Nose bleed
8.6. Allergies
8.7. Altered smell
9. Nose: Objective Data
9.1. Inspect symmetry, deformity, proportion, inflammation, sin lesions
9.2. Palpate if necessary
9.3. Assess patency of nostrils
9.4. Assess CN 1 (sense of smell)
9.5. Palpate sinuses
9.6. Nose Abnormalities
9.6.1. Nasal Polyps
9.6.1.1. Smooth, pale grey, avascular, mobile, non-tender
9.6.2. Deviated septum
9.6.2.1. Looks like a hump in nasal cavity
9.6.3. Perforated septum
9.6.3.1. Hole in the septum
9.6.3.1.1. Cocaine, chronic infection
9.6.4. Sinusitis
9.6.4.1. Acute, infected, inflamed sinus
9.6.4.1.1. Typically following upper respiratory infection
9.6.5. Eptaxisis
9.6.5.1. Nose bleed
9.6.5.1.1. Forceful coughing/sneezing, nose picking
9.6.6. Allergic Rhinitis(Hay Fever)
9.6.6.1. Abnormal immune response to antigens
9.6.6.1.1. Rhinorrhea
9.6.6.1.2. Itching of eyes and nose
9.6.6.1.3. Lacrimation(watery eyes)
9.6.6.1.4. Nasal congestion, sneezing
9.6.6.1.5. Allergic shiners
9.6.6.1.6. Nasal crease
10. Throat AKA Pharynx
10.1. Observe tonsils:
10.2. Color, moisture, are there crypts or exudate
10.2.1. Abnormal: Tonsillitis
10.2.1.1. Bright, red, swollen, white or yellow exudate on tonsils, and pharynx.
10.3. Tonsil grading
10.3.1. +1 visible
10.3.1.1. +2 Halfway between tonsillar pillars and uvula
10.3.1.1.1. 3+ Touching the uvula
10.4. Depress tongue with blade:
10.5. Gag reflex CN IX & X
10.6. Can stick out tongue and move side to side, coordinated speech? CN XII
10.7. Breath
11. Oropharynx/Throat abnormalities
11.1. Bifid uvula
11.1.1. Looks partly severed
11.1.1.1. May indicate cleft palate
11.1.1.1.1. May effect speech
11.2. Peritonsillar abscess
11.2.1. Occurs for untreated strep infection
11.2.1.1. Pus filled pocket
11.2.1.1.1. May require drainaige
11.3. Pharyngitis
11.3.1. Inflammation of the pharynx
11.3.1.1. Sore throat
11.4. Cleft Palate
11.4.1. Congenital defect
11.4.1.1. Failure of fusion of the maxillary process
11.4.1.1.1. Environmental factors
