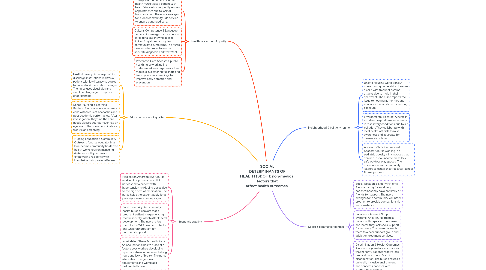
SOCIAL DETERMINANTS OF HEALTH (SDOH): non-medical factors that affect health outcomes.
von Charlotte Toombs
1. Education access & quality
1.1. Health Literacy: A nurse providing discharge instructions realizes a patient with low literacy struggles to understand medication dosages. The nurse uses visual aids and simplified language to improve understanding.
1.2. School Nursing & Learning Barriers: A school nurse assesses a child with frequent headaches and poor academic performance. After investigation, they find the child needs glasses but has never had an eye exam. The nurse coordinates a free vision screening.
1.3. Nursing Education & Community Outreach: A nurse educator in a low-income community holds free health workshops on managing diabetes and hypertension, empowering residents with knowledge to improve self-care.
2. Healthcare access & quality
2.1. Transportation Barriers: A home health nurse visits a patient with heart failure who frequently misses appointments due to lack of transportation. The nurse arranges for a local community ride service to ensure continued care.
2.2. Cultural Competence & Language Barriers: An emergency room nurse cares for a patient who speaks limited English and struggles to communicate symptoms. The nurse uses an interpreter to ensure accurate diagnosis and treatment.
2.3. Preventive Care Access: A public health nurse working in an underserved area organizes a free mobile clinic offering flu shots and blood pressure screenings to improve early detection and prevention.
3. Neighborhood & built environment
3.1. Unsafe Housing Conditions: A nurse making home visits observes a child with frequent asthma attacks due to mold in their apartment. The nurse reports the issue to housing authorities and educates the family on minimizing exposure.
3.2. Environmental Hazards: A nurse in an urban hospital sees an increase in respiratory conditions due to air pollution. They collaborate with local health officials to raise awareness and advocate for cleaner air policies.
3.3. Access to Safe Recreational Spaces: A nurse working in a pediatric obesity clinic notices that children in low-income areas lack safe outdoor play spaces. The nurse works with community leaders to establish a free after-school fitness program.
4. Social & community context
4.1. Social Isolation & Elderly Patients: A nurse caring for an elderly patient finds they have no family or friends for support. The nurse arranges for a community volunteer program to provide companionship and assistance.
4.2. Substance Abuse & Support Systems: An ER nurse treats a patient with repeated overdoses and learns they lack social support for recovery. The nurse connects them to a peer support group and addiction treatment services.
4.3. Discrimination & Health Outcomes: A nurse in a prenatal clinic notices that minority patients receive less prenatal care due to fear of discrimination. The nurse ensures a culturally inclusive environment and connects patients with supportive resources.
5. Economic stability
5.1. Medication Affordability: A nurse working in a primary care clinic notices that a patient with hypertension is skipping doses due to the high cost of medication. The nurse helps the patient apply for a prescription assistance program.
5.2. Food Insecurity: A community health nurse discovers that a pregnant patient is experiencing food insecurity, which affects fetal development. The nurse refers them to the WIC (Women, Infants, and Children) program for nutritional support.
5.3. Job-Related Stress & Health Risks: An occupational health nurse at a factory sees workers developing repetitive strain injuries due to long hours and lack of breaks. The nurse advocates for ergonomic adjustments and workplace wellness initiatives.


